Latest Update
 17 Apr 2023
17 Apr 2023 What Are Hutchinson Teeth?
Hutchinson’s teeth primarily indicate congenital syphilis, which happens when syphilis gets transmitted from the mother to the baby in her uterus or at birth.
This condition becomes distinctive when the primary teeth of the infected child start to sprout. The incisor and the molars develop to get a triangular shape. They might also be widely spaced or might the enamel might not have any structural integrity.
Hutchinson’s teeth are a part of what is commonly known as the “Hutchinson triad,” comprising the teeth, ears, and eyes.
This condition was christened after Sir Jonathan Hutchinson, a surgeon and syphilis expert from England, who practiced at the London Hospital in the late 1800s.
Hutchinson’s Triad
As mentioned, Hutchinson’s teeth have gotten the name from the British surgeon, who was one to link the condition to congenital syphilis back in 1858. He was also responsible for detecting two other symptoms that come with congenital syphilis, making what is popularly known as Hutchinson’s triad:
Hutchinson teeth (incisors that are notched or pegged in appearance)
Interstitial ocular keratitis (redness and inflammation of the cornea of your eye)
Deafness in the eighth nerve (sensorineural hearing loss)
Stay with us till the end to find out more about Hutchinson’s teeth, and what you can do to prevent this condition.
Causes of Hutchinson’s teeth
The main cause of Hutchinson’s teeth is exposure to syphilis, which is a bacterial infection, mostly sexually transmitted, before or during birth.
Sexually transmitted as it is, it is known to begin as a sore on the skin of the genitals, rectum, or mouth. This infection then broadens its horizon through the mucous membrane or through direct skin content with these sores.
Syphilis sores might be painless in the initial stages of the infection. More often than not, some people don’t even realize that they have had it even for years. Other symptoms that you might want to watch out for:
- a full-body rash
- flu-like symptoms (fever, muscle aches, sore throat)
- hair loss
These symptoms are ever transient by nature.
Babies are mostly the ones who have the sword hanging on them of developing Hutchinson’s disease and other symptoms if the mother has had syphilis for less than a couple of years. the risk intensifies if the infection hasn’t been treated prior to the 18th week of pregnancy.
The exposure might occur while the baby is still in the womb through the placenta or during the delivery of the baby itself.
Symptoms Of Hutchinson’s Teeth
While new-born babies might not exhibit the immediate signs of syphilis exposure in the beginning, the symptoms only start to develop with age. Affected children might experience the triad that includes:
inner ear issues (labyrinthine disease) that may cause deafness
eye issues (interstitial keratitis) that involve inflammation of the cornea
teeth abnormalities (Hutchinson’s teeth)
You might not even notice Hutchinson’s teeth until the child is about 5 years old or their permanent teeth begin to sprout- whichever happens earlier. This condition mainly targets the permanent central incisors and molars.
Specific features include:
- peg-shaped with a crescent-shaped notch
- thinning or discoloration of enamel
- smaller teeth
- widely spaced teeth
if you are not sure whether or not the child is exhibiting characteristics of Hutchinson’s disease, do check with your pediatrician, dentist, or orthodontist.
Treating Hutchinson’s Teeth
For treating Hutchinson’s teeth, one needs to first visit a pediatrician for diagnosis and medication
A lumbar puncture or a blood test is often recommended to confirm a case of syphilis. Options to treat it includes a shot of penicillin. If you are infected for more than a year, your child might also need additional doses.
A tooth damage that is already there cannot be undone with medical attention. The process to correct is called dental restoration.
There are several options for treating teeth:
Crowns
These are caps that the dentists attach to the teeth to bring them to normal size, shape, and overall functional order.
Bridges
These false teeth help fill in the gaps between the teeth. Bridges are also designed to fix bite issues and restore the natural smile and shape of the face.
Fillings
Dental fillings are a way to go to fill cavities or holes caused by weakened enamel and other ailments. They are a chemical amalgamation of the composite material (tooth color), silver or gold.
Dental implants
These are usually titanium metal post that is surgically attached to be used as a base for the crowns or bridges. Implants have to wait until the complete development of the jaw, which doesn’t happen till late teenage or early adulthood.
Consult your dentist to find out more about the kind of treatments that are best suited for your child. If you are worried about the expenses, then it is wise to contact your insurance company and talk to them and find out about your coverage.
Preventing Hutchinson’s Teeth
The best way to prevent Hutchinson’s teeth is to get your syphilis treated prior to getting pregnant or planning to get pregnant. You might not show any noticeable symptoms, so it is always wise to get tested before getting pregnant, for the sake of the baby.
To be specific, you might want to get tested for syphilis and other STIs if:
- If you have another STI. Having one puts you at greater risk of developing others.
- If you’ve not practiced safe sex and had multiple sexual partners since the last testing.
- If you’re pregnant or planning on becoming pregnant.
- It is imported to get rid of syphilis before the 16th or 18th week of pregnancy. Post that period, even if the disease is cured, the babies might still be born with irreversible deafness, eye issues, and bone and joint issues like Hutchinson’s disease itself.
Regular Dental Care
It is important that you take good care of your child’s precious pearls after they have sprouted, irrespective of their shape, size, and order. The American Dental Association recommends the following guidelines to take care of your teeth:
- Brush twice every day with a fluoride-based toothpaste.
- Floss between teeth daily, at least once.
- Limit sugary beverages and snacks.
- Consider using a mouthwash that also contains fluoride.
- See a dentist every six months or twice a year.
Conclusion
While Hutchinson’s disease is irreversible in nature, it is important to limit and treat the underlying cause- syphilis, to prevent other correlated health issues that might accompany it.
After the permanent set of teeth has sprouted, you can consult your dental health expert or your child’s pediatrician about the available cosmetic procedures to correct the appearance of the teeth to some extent.
Please get checked for syphilis if you’re pregnant or are planning to get pregnant, if you are suspicious that you might have been exposed to it. This helps you to seek early treatments to save the baby from getting infected.
 14 Apr 2023
14 Apr 2023 Complete Overview of Chipped Tooth
The hardened exterior of the structure of the teeth or the enamel is one of the strongest structures on your body. But it is obviously not indestructible. A strong and forceful blow or wear and tear in unnatural amounts can also lead them to chip. These incidents result in a jagged tooth surface that can be sharp, tender, and disfiguring.
Causes of Chipped Teeth
Teeth can chip for any number of reasons. Some common causes include:
Biting down on hard substances, like ice, hard candy, or a bone
Falls down or car and accidents
Playing contact sports without a mouthguard or safety devices
Grinding your teeth
Risk Factors For Chipped Teeth
It is only natural that weakened teeth are more susceptible to being chipped than stronger ones. Some of the factors that bring down the natural strength of the tooth are:
Tooth decay and cavities are known to eat away at the enamel. Large fillings also often tend to weaken teeth.
Teeth grinding can wear out the enamel.
Eating a lot of acid-producing foods, such as fruit juices, coffee, and spicy foods can break down enamel and leave the surface of teeth exposed.
Acid reflux or heartburn, two digestive conditions, can lead the stomach acid rising up into your mouth, which can damage tooth enamel.
Eating disorders or excessive alcohol use can lead to frequent vomiting, which in turn can produce enamel-eating acid.
Sugar produces bacteria in your mouth, and those bacteria can attack the enamel, weakening them in the process
Dental enamel anyway wears out with time, so if you happen to be 50 years or older than that, you are more prone to having a weaker or thinner enamel. In simpler words, it means, in ideal oral health conditions, the strength of the teeth is inversely proportional to your age. In one of the studies published by the Journal of Endodontics, nearly two-thirds of those with cracked teeth were over 50.
Which teeth are at risk?
Any weakened teeth are at risk of getting chipped. However, there is one study that shows that the second lower molar, is probably because of the fair amount of pressure it takes while chewing, and the teeth with dental fillings are most susceptible to chipping. That being said, intact teeth are also subject to chipping.
Symptoms of a chipped tooth
If the chip is minor or won’t show directly when you open your mouth, chances are you probably won’t even know that you have a chipped tooth. When you have a chipped tooth tough, the symptoms of a chipped tooth, however, might include:
Feeling a jagged or rough surface when you run your tongue over your teeth
Irritation of the gum around the chipped tooth.
Irritation of your tongue from “catching” it on the tooth’s uneven and rough edge
Pain or discomfort from pressure on the tooth when biting or chewing, which can be intense if the chip exposes the nerves of the tooth
Diagnosing a chipped tooth
Your dental health expert can easily diagnose or find out about a chipped tooth by running an inspection of your mouth. They will also ask you if you have experienced any relevant symptoms or events that might have caused the tooth to get chipped in the first place.
Chipped tooth treatment options
The treatment of a chipped tooth usually depends on three factors- severity, symptoms, and location. Unless the chipped tooth is causing non-negotiable inconveniences or is extremely painful, or is singlehandedly disrupting your meals and sleep, no additional medical attention will be necessary.
Having said that, you might still want to make an appointment with your dentist to avoid any chances of infection or save the teeth from any further damage. A minor chip usually takes a simple smoothing and polishing procedure to get fixed.
However, if the chip is extensive or severe, your dentist might recommend the following:
Tooth reattachment
If you still happen to have the broken fragment in your possession, soak it in a glass of milk to keep it moist, and the calcium in the milk will keep it alive. If you don’t have any milk at your disposal, tuck it safely in your gum, and make sure that you don’t swallow it.
Then, rush to the dentist as quickly as possible. They might be able to cement it back on the original teeth from where it broke off.
Bonding
A mixture of composite resin or place material, or porcelain (layers of ceramic) is cemented to the surface of the broken tooth and shaped to its form. Ultraviolet lights are then used to harden and dry the mixture. After drying, some more shaping is done until the material fits and looks exactly like the original tooth.
Bonds can sustain up to 10 years.
Porcelain Veneer
Before the veneer is attached, the dentist is required to smoothen the tooth enamel to some extent to make it easier for the veneer to attach itself. Usually, they shave away less than even a millimeter.
The dental health expert will take an impression of your tooth and will forward it to the lab to create a permanent veneer. After the permanent veneer is ready, the dentist will then bond it to permanently fix it to your tooth. Fortunately, enough, the veneer can easily last up to 30 years.
Dental Onlays
If the chip has affected only a portion of your tooth, your dental health expert might recommend a dental onlay, which is usually applied on the surface of the molars. However, if the damage is comparatively more significant, your dentist might have to recommend a crown. This procedure will need you to receive anaesthesia for the dentist to work on your teeth and make it easier for the onlays to get attached to the tooth.
Like veneers, the dentist will have to take an impression of the teeth and forward it to the lab to get an onlay created. Once the dentist gets hold of it, they will then cement it to the damaged tooth.
With the advancement in technology, some dentists can successfully create porcelain dental onlays right in their offices and cement them that very day.
Dental onlays can last for a very long time, almost for decades. However, a lot of it depends on your food habits, whether you eat a lot of the items that can cause the onlays to wear and tear faster than usual, and what tooth was affected, to begin with. The molars, for instance, will wear more easily because of all the pressure that It has to endure to chew the food.
Dental costs
The costs can vary depending on the part of the country you live in. The other factors include the tooth that has been damaged and the severity of it. However, if you are looking for a general estimation of the costs, you might want to look at the chart given below:
- Tooth planing or smoothing can cost you about $100.
- Tooth reattachment
This is comparatively pricy because you are going to have to pay for a dental exam, which alone will cost you between $50 to $350. However, considering the tooth reattachment procedure doesn’t require way too many materials, the charge excluding the cost should be minimal.
Bonding
$100 to $1,000, depending on the complexity involved.
Veneers or Onlays
The price for this procedure primarily depends on the materials used and the amount of preparation required before affixing the veneer or the crown, which lays anywhere between $500 to $2,000,
Self-Care For a Chipped Tooth
The chances are, that you will require a dentist to get a chipped tooth fixed, but there are other steps that your can follow to take care of your own teeth in the comfort of your home:
Place a temporary dental filling material, like a teabag, sugar-free gum, or dental wax over the jagged edge of the tooth to protect your tongue and gums from being injured by the sharp edges.
- Take an anti-inflammatory painkiller such as ibuprofen (Advil, Motrin IB) if you are experiencing any pain.
- Hold some ice on the outside of your cheek if the chipped tooth is causing irritation to the surrounding area.
- Floss gently to bring out any food caught between your teeth, which can cause even more pressure on your chipped tooth when you chew.
- Avoid using the chipped tooth to chew.
- Rub or apply clove oil around any painful gums to numb the area.
- Wear a mouthguard when you play sports to protect your mouth and teeth, or at night if you are habituated to grinding your teeth.
Complications Of Chipped Teeth
An infection might develop if the chip is extensive enough to affect the root of the tooth. Should that happen, the only recommended treatment is a root canal. Here is a list of symptoms that you might want to look out for:
- Pain when eating
- Sensitivity to hot and cold
- Fever
- Bad breath or sour taste in your mouth
- Swollen glands in your neck or jaw area
To Summarise
A chipped tooth is one of the most common dental injuries. In most case, it doesn’t usually cause any pain or inconvenience, even if it does it can be easily taken care of with the available dental procedures.
While it doesn’t usually categorize itself as a dental emergency, the sooner you get treatment, the better the chances of limiting any other associated dental problems. Recovery is generally fast once the dental procedure is initiated.
 14 Apr 2023
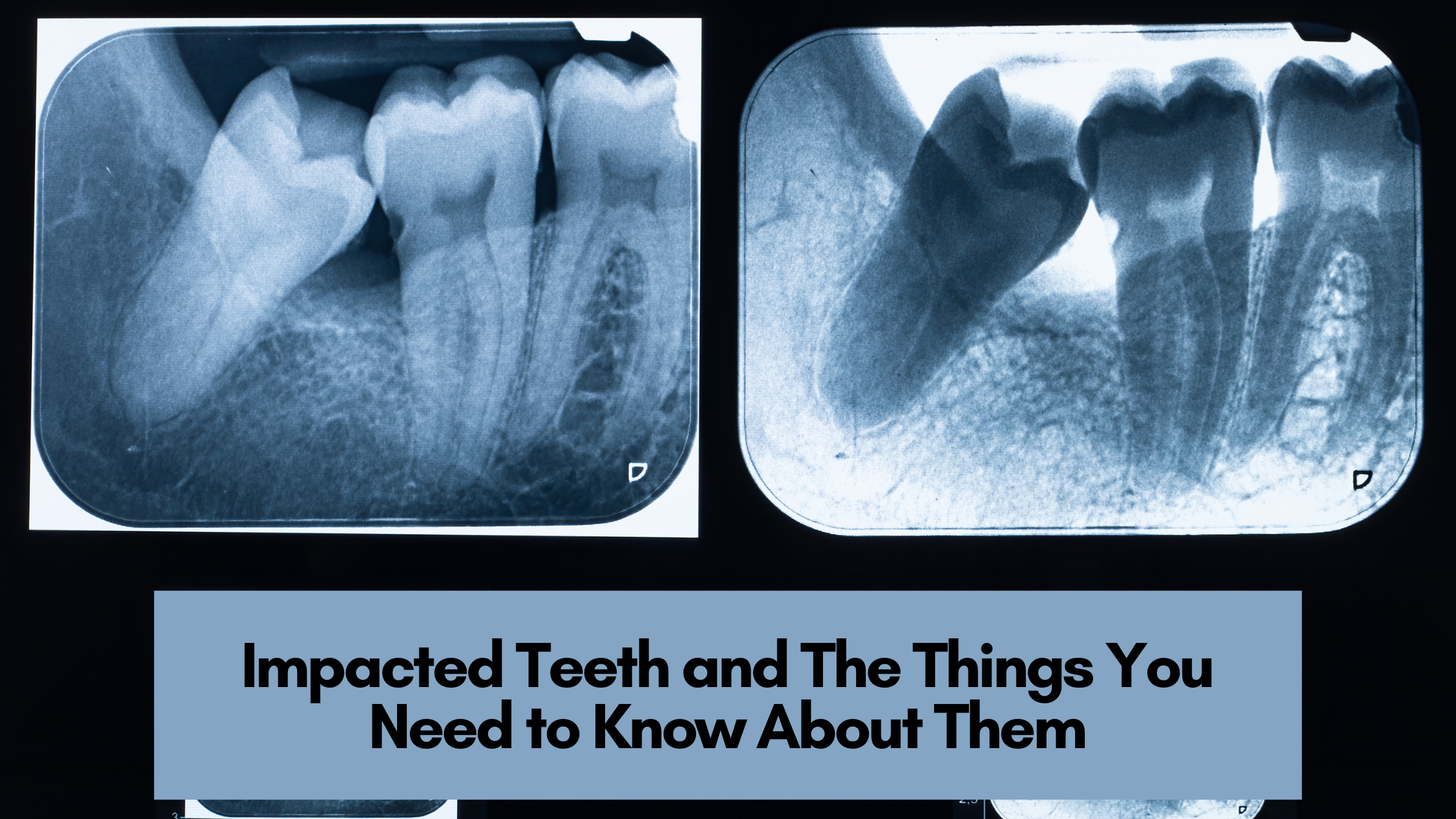
14 Apr 2023 Impacted Teeth and The Things You Need to Know About Them
What Are Impacted Teeth?
An impacted tooth is that tooth which some unknown reason has been blocked from popping out through the gum. Often the teeth might also be partially impacted, which means that they had begun to sprout but could not.
Sometimes, the impacted teeth can show no obvious symptoms and won’t be discoverable until a routine X-ray at the dentist’s office.
Symptoms Of Impacted Teeth
You might not even experience any signs or symptoms in some of the other cases, but an impacted tooth might lead to show certain obvious symptoms:
Red, swollen, or bleeding gums
Bad breath
A bad taste in your mouth
Difficulty opening your mouth
Pain when opening your mouth, or when chewing and biting
Symptoms may come and go.
What Causes an Impacted Tooth?
A tooth or teeth usually becomes impacted when your mouth doesn’t have space to accommodate all of them. This might be a result of genetics or an orthodontic treatment gone wrong.
Which Teeth Are Most Often Impacted?
Wisdom teeth are examples of typically impacted in nature. These typically sprout between the ages of 17-21 and are usually the last ones to grow.
By the time the wisdom teeth or the third molars start showing up, the jaw already stops growing. The mouth and the jaw hence might prove to be too small to accommodate all the wisdom teeth that would be coming in. Considering there is no specific need for wisdom teeth anymore, it is easier and more convenient to get them extracted if they happen to cause problems in chewing and talking. If you happen to have a smaller jaw, chances are that you might also have impacted wisdom teeth.
The second most common teeth to be impacted are the maxillary canines, also called the cuspid or upper eyeteeth. These teeth play a more significant role in your mouth, which is exactly why your doctor might recommend treatments that encourage these teeth to erupt instead of getting them removed.
How are Impacted Teeth Treated?
If you suspect to have an impacted tooth, try visiting your dentist as soon as possible without further procrastination. The dentist is most likely to take an X-ray of your mouth to find out if the symptoms that you have been experiencing were caused by impacted teeth. If the result is affirmative, they will then discuss the treatment and the plan of action with you.
The options to treat an impacted tooth include:
Waiting and Monitoring
If your impacted tooth is not causing any problem or showcasing any symptoms, your dentist might recommend you to go for the ‘wait and see ‘approach. When simply put, with this approach, the dentist with constantly monitor the impacted tooth instead of surgically extracting it, and waiting to see if it all becomes a problematic tooth.
This will be easier if you already are in the habit of visiting your dentist at regular intervals.
Surgery
Surgery will be recommended by your dentist if you are experiencing pain and unwanted side effects from an impacted tooth in your mouth, particularly when it is a wisdom tooth. The dentist might also recommend surgical extraction if the impacted tooth seems to cause harm to the other tooth in the mouth.
The tooth extraction surgery takes about only a day and the patient is allowed to go home the same day after the procedure is over. The procedure usually takes 45- 60 minutes, and the patient will have to undergo a process of local anesthesia prior to the procedure. The recovery too doesn’t take more than 7-10 days for the patient fully recover and get back to their normal lives.
Eruption aids
In cases when the canine teeth are impacted, eruption aids or medicines might be used to get the tooth to sprout out properly. Eruption aids might include braces, brackets, or by completely extracting baby or adult teeth that may be blocking the canines. However, these methods are most effective when performed on younger people.
If the desired eruption can’t be achieved, then the impacted tooth will either be extracted or be replaced with a dental implant or bridge.
Complications Of Impacted Teeth
An impacted tooth never breaks through the gums, you will neither be able to clean them, nor care for them. But, if your teeth happen to be partially impacted, they get way harder to clean. This in turn makes them more susceptible to dental or oral hygiene problems, including:
- Cavities
- Decay
- Infection
- Crowding of nearby teeth
- Cysts, which can damage the roots of nearby teeth or destroy the bone
- Absorption of bone or adjacent teeth
- Gum disease
Pain Management for Impacted Teeth
Over-the-counter medicines might be able to provide some temporary relief from the pain caused by an impacted tooth. Medicines like Aspirin have been found to provide effective relief for mild to moderate toothache. Having said that, it is not recommended to be given to children below the age of 18. This is because it can increase their risk for Reye’s syndrome, a serious condition.
Ice might also be helpful in reducing the inflammation, or you can also try rinsing your mouth with warm salt water, which is a time-tested method to provide relief from toothache.
If your pain is severe and these home remedies are not being of such help, visit your dentist to get yourself some prescribed pain reliever. Even if the home remedies make you feel better, it is always advisable that you visit your dentist to find a better solution. Using pain reliever medicines for a long span is extremely dangerous and if the impacted tooth doesn’t feel like it is going to feel better anytime soon, it is wiser to get it surgically removed or use other medical interventions.
Conclusion
Impacted teeth aren’t always the problem, and hence don’t require any medical attention at all. However, they require to be extracted surgically to prevent irritation, and infection, or to save the other teeth from being damaged by the impacted teeth.
Regular dental check-ups from an early age can help your dentist find out about impacted teeth before it gets out of hand, and begin the medical intervention if necessary.
 12 Apr 2023
12 Apr 2023 How Is Nose Pain Related To Teeth Pain?
A serious type of sinus infection can lead to many uncomfortable facial symptoms and this also includes tooth pain and oral health problems. A sinus infection occurs when certain viruses or bacteria infects the sinus linings. So what are these sinuses?
Sinuses are cavities which are filled up with air. Cilia which are the small hairs lines the sinuses. These small hairs helps in the movement of air, mucus, and bacteria or viruses through for filtration. The sinuses allows a route for air to flow and warms the air that enters through the nose. Sinuses are present in the skull. There are four different types of sinuses,
#a. Frontal Sinuses: These paired sinuses that are located above the eyebrows in the frontal bone that creates a person’s forehead.
#b. Sphenoid Sinus: These are the only unpaired sinus located in the head, the sphenoid sinus is located slightly deeper in the skull, located near the optic nerve and pituitary gland in the brain.
#c. Ethmoid Sinuses: This collection of air cells is in the ethmoid bone between the eyes and at the top of the nose. This bone separates the nasal cavity from the brain.
#d. Maxillary Sinuses: These are large, paired sinuses that are located behind the cheekbones and on either side of the nose. These sinuses are pyramid-shaped. Maxillary sinuses and are the largest sinuses in the head.
Without the sinuses, a person’s head would be heavier. These four different types sinuses also helps in determining the sound of a person’s voice, as their voice resonates or changes with air vibrations in the sinuses. Today in this article we would be looking into why a person experiences tooth pain which might related to the sinus infections and when one should visit a doctor in order to treat themselves.
At first you should clear one question in your mind weather an infection in sinus causes tooth pain?
Can A Sinus Infection Lead To Tooth Infection?
Well, a sinus infection can lead to dental pain, and as per studiesthe most common sinus infection site which leads to causing dental pain is the maxillary sinus. The sinuses, teeth, and gums all of them share similar nerves that can transmit pain signals.
Inflammation that occurs due to sinus infection or any dental disease can press on the nerves, and this leads to pain. In that case a person might interpret these signals as dental pain.
Can A Dental Infection Cause A Sinus Infection?
Just like a sinus infection leads to dental pain, similarly dental infection too can lead to end up causing sinus infection. A dental infection can also lead to sinus infection. Studies conducted in 2012 have shown that nearly 40% of chronic maxillary sinus infections had occurred due to dental infections.
Whereas older studies have estimated this amount was about 10%, but advances in imaging, such as CT scans, have revealed dental infections as the most common underlying cause.
As it is seen that the back portion of the teeth is close to the maxillary sinuses, several infectious organisms can travel down to these cavities. A person with this infection type will have maxillary sinus infection symptoms. They may also have the following risk factors which are related to their teeth such as history of jaw or dental pain, history of or current dental infection, or history of endodontic, oral, or periodontal surgery, especially tooth extractions.
If infection of this type takes place then in order to treat it there is requirement of antibiotics and treatment of the underlying infection in the tooth or teeth. And doing this would help in the reduction of chances of the infection returning again.
Dental problems can end up causing pain or pressure in some of the sinus areas. This may include sinus-like pressure or an achy feeling in the upper, back teeth. If anyone experiences this type of dental discomfort, then in that case you may need to visit both the dentist and the doctor to determine the root cause of the pain in order to treat it. But if the pain is in the lower teeth or towards the front of your mouth, it’s not likely you have a sinus type of infection.
By now you have known how sinus infection can lead to dental infection and does dental infection leads to tooth infection.
Sinus Toothache Vs. Regular Toothache
If you are feeling pain then you should visit doctor in order to get the treatment done, the doctor would look at the different symptoms and then would help to diagnose the toothache which had occurred due to sinus infection or if there is any other dental problem. Below mentions are causes that can lead to causing sinus infection.
#a. interference with a person’s sense of smell
#b. one-sided nasal obstruction, or a stuffy nose
#c. runny nose, typically on one side
Whereas the signs that may be different from sinusitis and could indicate a dental problem include:
#a. dental pain with temperature changes, such as when eating or drinking something cold or hot
#b. facial swelling
#c. gum swelling near a tooth
#d. pain near a tooth that has dental work
What Are Some Of The Other Symptoms Of Sinusitis?
A person who has sinusitis will usually have a history of a recent upper respiratory tract infection, and most commonly cold. They would start to recover from the cold and may then start experiencing sinusitis symptoms.
These symptoms includes:
#a. discharge from the nose
#b. facial pain
#c. nasal congestion
Whereas some people experience chronic sinusitis because their sinuses do not drain well. Their symptoms can last 8–12 weeks. Those who have chronic sinusitis are less likely to experience dental pain or facial pain than those have acute sinusitis.
How Is Treatment Of Sinus Infection Done?
The treatment of sinus infection can be done both at home and through medical treatment too.
Treatment for sinus infection
A person can sometimes treat their sinus infection at home with the help of home remedies in order to get relief.
#1. Nasal irrigation:
Irrigating the nasal cavity with the help of warm or room-temperature saline solution is done in order to promote mucus drainage. One can put a warm saline solution in a 10- or 20-milliliter of water syringe and slowly instill this into the nasal passages while leaning over a sink or bowl.
One need to make sure that the solution should run down the face, and not back into the sinus passages or throat. The person should ensure that the saline solution is not hot and make it with distilled, sterile, or previously boiled water, as because tap water might not be clean.
#2. Topical decongestants:
Utilizing the topical decongestants, such as ephedrine, can lead to allow more air to flow through the sinuses. But a person should not use decongestants for more than 7 days.
#3. Warm compresses:
Placing warm compresses over the sinus areas may lead to reducing pressure. Examples include over the forehead and on either side of the nose.
#4. Rest and fluids:
By resting and drinking plenty of water, people will help thin their nasal secretions can do their treatment.
Medical treatment
An exception to treat sinusitis at home is when a person has a fever, or the infection seems to have spread beyond the sinuses, such as into the other organ like ears.
Someone who has pus-filled nasal discharge might also get benefit if they take antibiotics. Treatment for infectious sinusitis is amoxicillin. If a person is allergic to amoxicillin, then in that case a doctor may prescribe doxycycline or clarithromycin.
If a person is continually experiencing sinusitis that affects their breathing and quality of life, then in that case their doctor may recommend sinus surgery in order to do the perfect treatment. Surgery can lead to widening sinus passages in order to reduce the likelihood of infection and irritation that might occur.
When One Should See A Doctor For Treatment?
A person should see a doctor if they experience the following symptoms mentioned below:
#1. Severe sinus pain
#2. Fever that lasts more than 3–4 days
#3. Severe dental pain
#4. Inability to eat or drink related to dental or facial pain
If the symptoms lasts more than 10 days without any improvement, then in that case the person should visit the doctor for getting the treatment done. If a person is experiencing multiple sinus infections over the course of a year, then in that case they should seek medical treatment. A doctor can advise them on how to reduce the risks of having chronic infections and maintain a healthy lifestyle to treat the problem.
Conclusion
Toothache might be a symptom of an acute sinus infection. However, a dental infection can also lead to a sinus infection resulting to several other problems.
Due to this reason, a person should not ignore their symptoms if they persist beyond a few days or worsen, and they should seek medical attention for treating themselves.
 11 Apr 2023
11 Apr 2023 Everything About Tongue Cancer
What Is Tongue Cancer?
Tongue cancer is a type of head and neck cancer, it usually develops in the squamous cells which is located on the surface of the tongue. This in turn leads to tumors or lesions and later develops into cancer. Tongue cancer begins when there is a growth of abnormal cells that begins to divide and grow in a much-uncontrolled way.
Tongue cancer is a type of head and neck cancer. This cancer begins when there is a growth of abnormal cells that begins to divide and grow in an uncontrolled way. Tongue cancer usually develops in the squamous cells which are located on the surface of the tongue.
What Are The Causes Of Tongue Cancer?
There are several reasons which tongue cancer occurs, the primary reasons for the causes of tongue include:
#1. Poor nutrition: Eating a diet low in fruits and vegetables and sources of vitamin A
#2. Weakened immune system
#3. Some genetic syndromes
#4. Graft-versus-host disease
#5. Lichen planus, an inflammation of mucous membranes
#6. Using Marijuana.
What Are The Symptoms Of Tongue Cancer?
The most common sign of tongue cancer is an ulcer, sore or bump that occurs on the tongue and this bump doesn’t heals or fades away and it might also bleed easily. Tongue cancer might be a painful thing as one might feel that their tongue is burning. Some of the common symptoms of tongue cancer includes:
#1. White or red patch on the tongue
#2. The thickened area on tongue
#3. Persistent discomfort or pain in the tongue and/or jaw
#4. Burning sensation in the tongue
#5. Numbness in tongue
#6. Bleeding from the tongue that’s not from an injury
#7. Lump in your neck
#8. Sore throat or a persistent feeling that something is caught in the throat
#9. Swallowing or chewing problems
#10. Difficulty moving tongue or jaw
#11. Trouble speaking
#12. Bad breath
#13. Weight loss
#14. Fatigue
#15. Mouth numbness
#16. Dark patches on the tongue
#17. Lump on the tongue that doesn’t goes away
#18. Pain while swallowing
#19. Highly sore throat
#20. Lumps on the tongue.
What Is The Diagnosis Of Tongue Cancer?
While diagnosing tongue cancer the doctor is first going to perform a visual and physical examination of your tongue, throat, and neck. A biopsy of the suspect ulcer or tumor would be done to gain a small tissue sample for laboratory analysis of its cells.
Biopsies of oral tongue tumors can be done under local anesthesia, while growths in the base of the tongue may require the use of a laryngoscope or a fine-needle aspiration in some cases and may require general anesthesia.
In addition, a computed tomography (CT) scan of the neck may provide more information about the location of the tumor and its size, as well as the condition of lymph nodes that drain the area. A contrast medium may be injected into a vein in order to improve visualization during the scan.
Even special X-rays, such as CT scans, MRIs, or Panorex, might also take place. (A Panorex is an x-ray that shows the full upper and lower jaw, plus the sinuses.) These imaging tests provide more details about cancer. If cancer is found in your tongue, these images can show how deep the cancer is and if it has spread.
Other than that there are two types of tests too that are conducted one is a toluidine blue dye test and the other one is a fluorescent light test.
In the toluidine blue dye test the doctor or dentist coats the inside of the mouth in dye. The dye turns a darker blue if it spreads over an abnormal area then it indicates a problematic situation. Whereas in fluorescent light test the dentist or doctor shines a special light into the mouth. The light will reflect differently off any abnormal areas as the test is conducted.
What Are The Risk Factors That Leads To Tongue Cancer?
Tongue cancers occurs due to various reasons, but the major reasons are heavy smoking and high consumption of alcohol and these are the two most significant reasons due to which one can develop tongue cancer. Studies have also suggested that people who smoke and drink heavily are 15 times more likely to develop oral cancers than other people.
However, in recent years, it is also seen that a higher number of younger people and females have started developing tongue cancer. Experts believe that this may, at least in part, correspond to a rise in HPV-associated oropharyngeal squamous cell carcinoma cases. They continue to look at other potential risk factors that may explain the shifting demographic. While the other known risk factors include.
#1. Chewing tobacco and smoking
#2. Eating a diet low in fruit and vegetables and high in red meat or processed foods
#3. Having human papillomavirus (HPV) infection
#4. Having a family history of tongue or mouth cancers
#5. Having had previous cancers, particularly other squamous cell cancers
#6. Being male, as oral cancer is twice as common in males as females.
How Is The Treatment Of Tongue Cancer Done?
The treatment of tongue is done depending on:
#1. The stage of your cancer
#2. The part of the tongue where cancer took place.
#3. The general health of the patient.
What Are The Stages Of Tongue Cancer?
The stage of tongue cancer tells it clearly how big the problem is, and whether the cancer has spread or not. The stage of cancer helps your doctor to identify which treatment you need.
The stage of your cancer tells you how big it is and whether it has spread. It helps your doctor decide what treatment you need. Well, the stage of cancer depends upon:
#1. How far your cancer has grown into local tissues
#2. Whether it has spread to nearby lymph glands
#3. Whether it has spread to any other part of the body
Doctors use different types of staging systems in order to detect cancer. The staging system they use for you depends on where your cancer has started. Tongue cancer that starts in the front two-thirds of your tongue (oral tongue) is staged as a mouth cancer.
How Do Doctors Treat Tongue Cancer?
People with tongue cancer will usually require surgery to remove the cancerous tissue. Surgeons can generally remove smaller tumors in a single operation.
Multiple and more complicated operations may be necessary if larger tumors are present or cancer has spread. The surgeon may also need to remove part of the tongue. If this is the case, they will attempt to rebuild the tongue using skin or tissue from other parts of the body.
Surgery that involves the removal of part or all of the tongue is called a glossectomy. Although doctors will attempt to minimize the damage to the mouth during the procedure, some side effects are inevitable.
Glossectomy can have an effect on speaking, eating, breathing and swallowing.
In addition to that, some people may have radiation therapy or chemotherapy treatment in order to kill any cancerous cells that remain and doing this it can prevent further spreading of the cancer.
 11 Apr 2023
11 Apr 2023 Hyperdontia and Everything You Need to Do About It.
Hyperdontia is a medical condition when way too many teeth grow in your mouth. This condition is also called Supernumerary teeth. The additional teeth usually grow right behind or very close to your usual primary or permanent teeth.
What is Hyperdontia?
Hyperdontia is a medical condition that leads to the growth and generation of way too many teeth inside the mouth. These are also called supernumerary teeth. These teeth tend to pop up from anywhere in the curved areas, where teeth attach themselves to the jaw. These places are also referred to as dental arches.
The first 20 teeth that develop when you were a child are known as the set of primary or deciduous teeth. The 32 adult teeth that take their place in the future, is called a set of permanent teeth. You might have an additional number of primary or permanent teeth owing to hyperdontis, but cases with extra primary teeth are more commonly found.
What are the symptoms of Hyperdontia?
The primary sign and symptom of hyperdontia is the growth of additional teeth exactly behind or very close to the usual primary or permanent set of teeth. These teeth are generally found in adults. Men are twice as likely to struggle with hyperdontia than women.
Additional teeth are classified based on their shape or location in the mouth.
The Shapes of extra teeth include:
Supplemental.
The tooth is almost similarly shaped to the type of tooth that it grows up close.
Tuberculate.The tooth has a tube or barrel-like structure.
Compound odontoma
The tooth happens to be made up of umpteen smaller tooth-like structures that grow very close to each other.
Complex odontoma.
Instead of a single tooth, an area or a structure comprising tooth-like tissue grows in a disordered cluster-like formation.
Conical, or peg-shaped.
The tooth has a flat and wide base and a narrow pointy top, making it appear sharp.
Locations of extra teeth include:
Paramolar.
An additional tooth sneakily grows towards the back of your mouth, next to or really close to the molars.
Distomolar.
An additional tooth develops and grows in the same line with your other molars, rather than around them.
Mesiodens.
An additional tooth grows around or behind the incisors, the four flat and big teeth located at the front of the mouth, primarily used for biting. This is one of the most common categories of additional teeth among people struggling with Hyperdontia.
Hyperdontia is not usually painful. Having said that, an additional tooth or teeth might exert some additional pressure on the jaws and the gums, often leading them to swell or become sensitive and painful. Overcrowding caused by Hyperdontia might also make your permanent teeth appear crooked.
What causes Hyperdontia?
The exact reason behind the causation of Hyperdontia is not yet conclusively known, it is likely to be associated with multiple hereditary conditions including:
Gardner’s syndrome.
A rare genetic disorder that causes skin cysts, skull growths, and colon growths.
Ehlers-Danlos syndrome.
It is an inherited medical condition that causes loose joints to easily dislocate, bruises skin like that of a peach, scoliosis, and painful muscles and joints.
Fabry disease.
This syndrome causes an inability to sweat, painful hands and feet, a red or blue skin rash, and abdominal pain.
Cleft palate and lip.
These birth anomalies are known to cause an opening in the roof of the mouth or upper lip, which causes trouble eating or speaking, and even ear infections.
Cleidocranial dysplasia.
This condition causes anomalies in the development of the skull and collarbone.
How is Hyperdontia diagnosed?
Diagnosing Hyperdontia is no rocket science and can be easily detected if the extra teeth have already started to show up. Even if they have not started being visible, they will still be detectable during your regular dental x-ray. Your dental health expert might also require a CT scan to get a better look at the insides of your mouth, jaws, and teeth.
How is Hyperdontia treated?
Most cases of hyperdontia don’t usually require any medical treatment. However, some cases do require special medical attention or the surgical extraction of the extra tooth or teeth. Your dental health expert is most likely to recommend the extraction of the additional tooth or teeth if you,
- Have an underlying genetic condition causing the extra teeth to appear
- Can’t chew properly or your extra teeth cut your mouth when you chew
- Feel pain or discomfort due to overcrowding
- Have a hard time properly brushing your teeth or flossing because of the extra teeth, which could lead to decay or gum disease
- Feel uncomfortable or self-conscious about the way your extra teeth look
If the extra teeth are starting to affect your dental hygiene or other teeth — like delaying the eruption of permanent teeth — it’s best to remove them as soon as possible. This will help avoid any lasting effects, such as gum disease or crooked teeth.
If the extra teeth only cause you mild discomfort, your dentist may recommend taking nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil, Motrin) for pain.
Are there any complications related to Hyperdontia?
The extra teeth can cause mild to severe complications. Some examples are – overcrowding and decay. Additionally, if the tooth tissue is left behind, it can mutate into a cyst or tumour. Complications related to Hyperdontia include:
- Gap between teeth
- Overcrowding or crooked teeth
- Delayed eruption of permanent teeth
- Pain and inflammation
- Infections, such as gingivitis
- Impaction of permanent incisors
- Abnormal root formation
- Cystic lesions form around the teeth
If you come across or happen to notice extra teeth that are not in the same line with the surrounding teeth, or is causing you unnecessary discomfort, try checking with your dentist.
Living with Hyperdontia
Most people with hyperdontia don’t usually require any additional medical attention. Some people however need to get their extra teeth removed to avoid further inconveniences. Do check with your doctor if your condition leads to swelling gums, pain, or discomfort in your mouth.
 07 Apr 2023
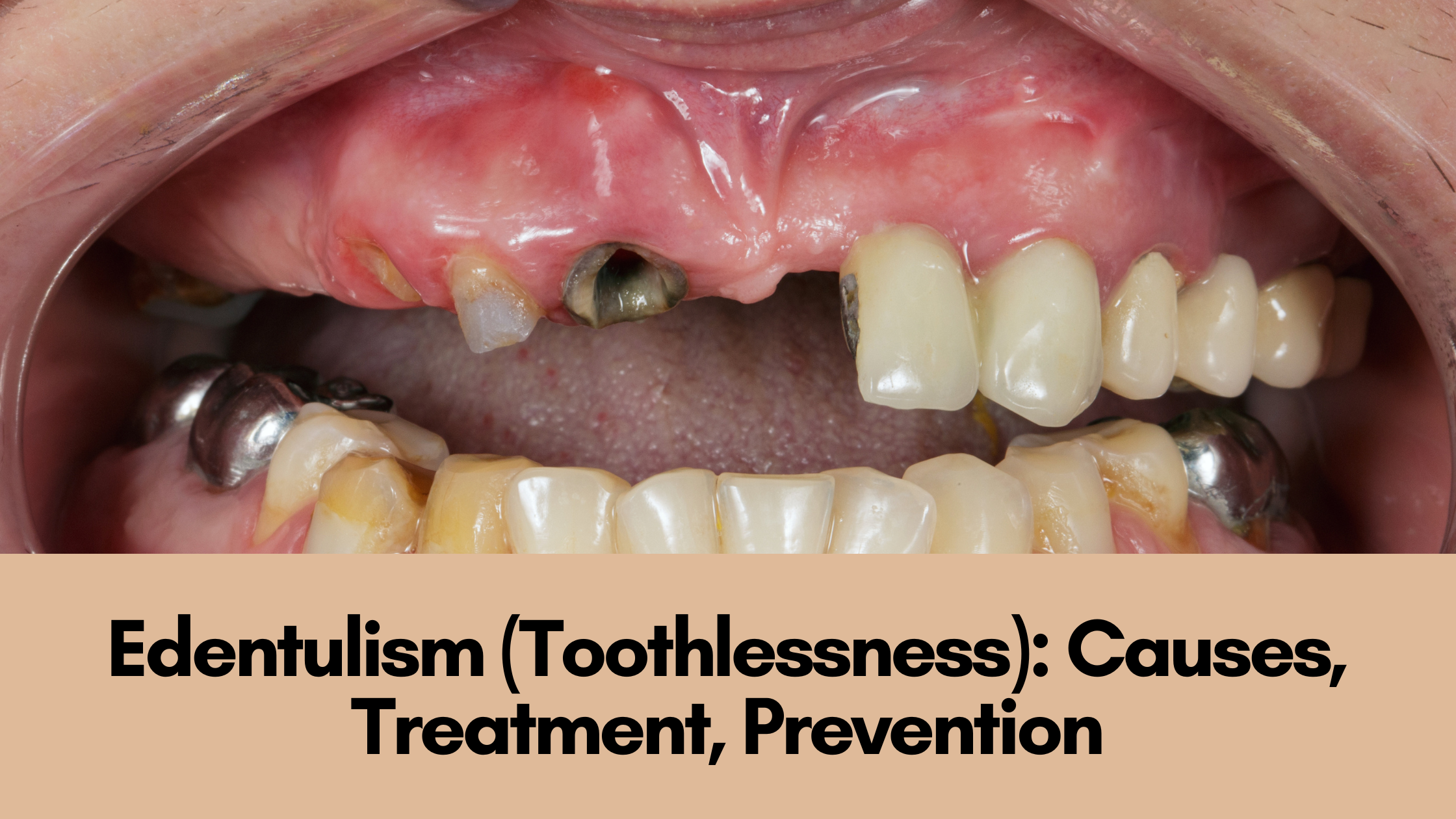
07 Apr 2023 Edentulism (Toothlessness): Causes, Treatment, Prevention
Edentulism, otherwise known as complete tooth loss is an oral condition where the patient loses some of their teeth or all of their teeth. Missing teeth is a serious issue and is known to have detrimental impacts on overall health because it makes it hard for the patient to chew the food, which later hampers the process of digestion.
This condition is primarily found among people in the United States, among adults, and people who are 60 years or older. If we were to look at what the American College of Prosthodontics had to say about this condition, we know come to know that more than 36 million people struggle with this condition in America.
There are even some isolated cases of edentulism among younger children- especially among the ones who fail to maintain proper dental health or an oral hygiene regimen. Besides being the first step in the process of digestion, teeth also define and structure the facial appearance of a person.
Types of Edentulism
Edentulism can be further divided into two main categories that can affect a person- partial and complete.
Partial Edentulism
This refers to a condition where individuals lose some of their natural teeth. the condition of partial tooth loss occurs comparatively more on the upper jaw than on the lower jaw.
Complete Edentulism
People who struggle with complete edentulism happen to lose all of their natural teeth to the condition. This too can be further classified into four subcategories depending on the diagnostic findings, where Class 1 represents an uncomplicated clinical situation and Class IV signifies a complex clinical case.
Prevalence of Edentulism
In spite of witnessing a significant plunge in the past decade, edentulism is still pretty common. The Centre for Disease Control and Prevention observed that from 2011 to 2016, one out of 6 adults 60 years and older lost one or more teeth. Adults over the age of 65 are the ones who were mostly affected by tooth loss as compared to younger adults.
According to the surveillance report presented by the Centre for Disease Control and Prevention, it was found out that almost 17% of the older population struggles with edentulism. Among those younger than 65, the rate is 4 percent.
Causes
Tooth loss can be directly linked to the bacteria that enhance it by causing oral infections. However, there might be other factors responsible for this condition:
Trauma
One of the primary causes of accidental tooth loss might occur when a person experiences a blunt force, perhaps during an injury caused in any possible situation. Such sudden force is sufficiently capable of causing dental dislodgement, and can even hurt the jaw bones sometimes. Dental trauma is one of the main reasons for tooth loss among children.
Dental caries
Dental decay or dental caries causes holes in your teeth. These holes when left unattended or untreated can lead you to cause irreversible dental damage, compelling your dental health expert to uproot them to save the other teeth from further damage.
Periodontal diseases
Periodontitis, also known as gum disease, attacks the gums. This condition attacks the gums and the jaw bones hampering their natural function. Where long-term periodontitis goes untreated, it can lead up to edentulism.
Low educational level
People who don’t have access to basic education or don’t have any educational background often are not aware of the importance of maintaining a proper oral health regimen, which is important in preventing the loss of teeth.
Poor oral health
Not maintaining a proper dental care regimen is one of the major red flags and can cause tartar and plaque build-up or other oral health diseases, which might eventually lead to edentulism over time. It has also been scientifically proven that even coronary diseases can be directly linked to a bad oral health condition.
Low income
Frequent trips to the dentist’s chamber can be really expensive, especially if you are not covered under a dental insurance plan. People with a lower income often cannot afford to visit trips to the dentist as frequently as they need to, or often do not visit them on purpose to save some extra bucks. This can lead to dental disorders and eventual edentulism.
Poor diet
If your diet includes more sugary food items and beverages than clean fruits and vegetables, there are chances that you might have to struggle with gum disease, which might lead to loss of teeth when left untreated.
Osteoporosis
Osteoporosis is a condition that affects bone density, making them weak and leading to fractures. This condition affects the long and the short bones, including the one supporting your jaw structure. It leads your jaw bones to become less dense, resulting in eventual tooth loss.
Risk Factors
These are some common factors that might heighten your chances of struggling with tooth loss. They are:
Age
Your tooth enamel is likely to wear out with age. Besides that, the gums holding and supporting your teeth also begin to recede, making your teeth long more exposed and longer. You also happen to experience a reduction in the amount of saliva production in your mouth. All of these factors are like to increase your chances of suffering from edentulism at a later stage in your life.
Smoking
The percentage of tooth loss among smokers is much higher than among non-smokers. Gum diseases can be directly linked to smoking, according to the CDC. If the disease goes untreated and is allowed to progress, it might also affect the jaw bones and their integrity to hold the teeth in place.
Gender
As weird as it might sound, women are more susceptible to tooth loss than men. It is because the hormonal changes that they undergo indirectly impact their oral health situations. During menopause, some of the hormones like estrogen decrease, leading to a loss of the jaw bone making women slightly more susceptible to osteoporosis.
Impact on Oral and General Health
Lack of adequate dentition or tooth loss can have detrimental and undesirable impacts on the general and overall health conditions of a person. It is known to impact the oral health of a person in the ways listed below:
Impaired mastication
As discussed earlier, a lack of the appropriate number of teeth can hamper the digestion process by making it difficult to chew or bite the food. This severely affects even your diet, because you are going to have to be picky and selective and choose the ones that are easy to break and gulp down.
Modifies the physiology of the mouth
Edentulism is also known to weaken the upper and lower jaw bones. It also leads to a condition that causes the breaking down of the jaw bone that remains after the teeth removal, also scientifically called residual ridge resorption. It leads to a reduction in the size of the jaw containing the sockets to hold the teeth in place.
Determinant of oral health
Saliva plays multiple functions inside the mouth, one of them being protective in nature. When the mouth starts to produce lesser amounts of saliva, the safety of the mouth and the body is compromised also possibly leading to tooth loss.
Other Issues with Tooth Loss
Just when you thought you knew all the problems that can follow tooth loss, we have some more for you:
- Reduction in the intake of healthy and clean foods such as fruits and vegetables.
- Increases the chances of pancreatic cancer and ulcers concerning the digestive system.
- It may lead to noninsulin-dependent diabetes.
- Causes sleep apnoea, a breathing disorder experienced during sleep, might also be fatal.
Furthermore, people with edentulism usually prefer eating fast foods that take much lesser effort to chew. These food items are known to contain high cholesterol levels, which can lead to obesity and coronary disease.
Prevention
Preventing tooth loss might not always be possible. But there are obvious methods that can help you keep gum diseases and other oral health diseases at bay, which will delay the process of tooth loss before time:
- Brush your teeth at least twice a day.
- Floss your teeth at least once a day.
- Use dental sealants to prevent tooth decay.
- Avoid, and if possible, quit smoking as this leads to gum disease.
- Include calcium and vitamin D into your diet to form strong bones.
- Visit the dentist every six months
Treatment
Dentists take to different pathways to treat edentulism, based on the severity of the tooth loss. With people with partial edentulism, dental health experts take to replace the lost teeth with new partial dentures. They also use implant-supported prosthetics or artificial tooth roots which are screwed down onto the jaw bones. This contains a single artificial tooth attached to them.
However, when it comes to people struggling with complete edentulism, dental health experts are likely to present the patient with two choices, dentures or a bridge.
Dentures
These are a set of false teeth used to replace the old and the natural ones. You can either get it permanently attached or make them removable. In the case of complete edentulism, the dental health expert is most likely to use full dentures.
Tooth bridge
It is designed to be made with a metallic frame with artificial teeth attached to it. This dental health expert will fix the bridge to the mouth, where the original teeth used to previously exist.
Facial Support and Aesthetics
A set of teeth is multifunctional, one of which is to provide structural support to the face. The structural support provided by the teeth and jaw bones enhances the facial appearance of a person. The lips, for instance, are supported by the frontal teeth.
The cheeks of an edentulous patient appear sunken and affect the facial appearance of the patient. again, without the teeth present, the tongue muscles tend to broaden and fill the mouth, often hampering speech. The broadened tongue can also make it difficult for a person to use dentures. The good news is that you can get it corrected with aesthetic reconstruction. It requires the use of a facial scanner to visualize and predict the normal facial appearance of a person.
 07 Apr 2023
07 Apr 2023 Bad Breath from Stomach Ulcers – Symptoms and Treatment
If you happen to experience bad breath regularly, stomach ulcers might be a probable cause. The subsequent stomach ache is usually known to stem from an infection of H. pylori, a common strain of bacteria that can be directly linked to gum diseases or periodontal diseases and bad breath.
Stomach ulcers mostly require a strong and consistent dosage of antibiotics and various other steps to reduce the amount of acid inside the stomach and the body. You can easily save yourself all the trouble if you eat well, take some time out to relax, reduce the consumption of alcoholic beverages and quit smoking, and avoid excessive or unnecessary use of common anti-inflammatory drugs.
What Are Stomach Ulcers?
Stomach ulcers can easily be defined as open sores or lesions that form on the inner lining of the small intestine or the stomach. They are also called peptic ulcers. They develop over time and might also occur in isolation or clusters.
As we have already mentioned, stomach ulcers are known to be caused by Heliobacter pylori, or H. pylori strain of bacteria. This strain attacks and weakens the inner lining of the stomach. Should this happen, the tissues of your stomach become vulnerable to the acid present in your system, and the ulcers start to take shape in response to this constant and increases exposure.
People usually have H.pylori bacteria lying dormant inside their systems. This is not even a matter of concern, because this strain of bacteria is usually harmless. However, only a tiny portion of people tend to develop ulcers as a response to exposure to the acid.
Stomach ulcers might also come into existence from the medications that you take. Many anti-inflammatory medicines, also known as NSAIDS, are formulated to inhibit the usual mechanisms your body employs to save the inner lining of the stomach from the acid inside it. Acids that can lead to the formation of stomach ulcers.
The urea breath test is an easy process used by professional doctors to test the presence of the H.pylori virus. The patients are first required to breathe inside a special medical bag that is used to measure the presence of carbon dioxide. They are then given a chemical solution containing urea. The virus reacts to the presence of urea by breaking it down into carbon dioxide. If the second bag contains significantly more carbon dioxide when compared to the first bag, the H.pylori content in your system is concerning. The doctors then mark you as infected by the bacteria and your chances of getting an ulcer are pretty high.
There are other methods used by doctors, which seem to be comparatively more invasive in nature. These methods include endoscopy or biopsy, to derive a more concretized result to detect the presence of ulcers. However, these methods are only put to use when the results derived from the urea breath test are not as conclusive as they should have been.
Why Do Ulcers Affect Your Breath?
The reason behind the bad breath is not the ulcer, it is the H. pylori bacteria that is causing the breath to smell bad. Studies show that people suffering from halitosis, otherwise simply known as bad breath, are more likely to have H. pylori in their system than people in control groups. Having said that, not everybody who is infected struggle with bad breath or halitosis, the exact connection between these two are yet to be completely discovered. This bacteria is so versatile in nature that it can also be connected to periodontal or gum diseases, which might also be held accountable for the causation of bad breath.
The presence of stomach ulcers itself indicates that you might have extra amounts of acids in your body, which might also lead you to struggle with additional inconvenient medical conditions like acid reflux, which adds to bad breath.
It is important that you don’t let your stomach ulcers go unattended. Seeking proper medical help will help control stomach ulcers and reduce the acid levels in your stomach, which in turn will reduce the signs and symptoms of these conditions as well.
Try making your gut healthier, because a healthy gut will only help you curb the bad breath in your system. Probiotics can restore the acid balance in your digestive system, so you’re less likely to suffer some adverse effects or prevent it from getting any worse.
Signs and Symptoms of Bad Breath from Ulcers
Bad breath is not the only indicator of a possible ulcer formation in your stomach. Many other symptoms might help you confirm if it is the ulcer that is causing all the inconvenience:
- Burning or gnawing pain in your abdomen
- Indigestion
- Heartburn
- A loss of appetite
- Unintentional weight loss
- Fatigue
- Generally feeling ill
There are certain symptoms of peptic ulcer that might also hint at some way graver than you can imagine, including complications like internal bleeding. When you let these symptoms go unattended, things might go way out of hand and might cause irreversible damage, possibly even death. You might want to immediately seek medical help if you notice or experience the following:
Vomiting blood (this may be ordinary red blood or dark and grainy-looking like coffee grounds
Passing dark, sticky stools that resemble tar
Feeling a sudden and sharp pain in your abdomen that worsens over time
Treatment Options
When stomach ulcers play the antagonist in your health scenario and cause you to have bad breath, only taking care of your oral health and dental hygiene will not possibly suffice.
If you are sure that all the discomfort and inconvenience are caused by the H. pylori bacteria, it is advisable that you seek medical help from an expert to get the bacteria out of your system. Make sure that you take the entire course of the medicine as prescribed by the doctor, even if you are feeling better before the course ends. Not finishing the whole course might cause the bacteria to resurface and cause infection, which will only take you back to square one.
If there is some other reason behind your ulcers, or if your case is slightly more serious than it should have been, your doctor might also prescribe proton pump inhibitors (PPIs), cytoprotective agents, or acid blockers to bring down the acid content in your stomach. They may also recommend that you take an antacid in the future to relieve the discomfort of your symptoms.
After your stomach ulcer has been taken care of, it is important that you take good care of your dental health and oral hygiene, and see your dentist at regular intervals. This will help you keep all kinds of periodontal diseases in your mouth and also freshen your breath in the process.
How Do You Prevent Ulcers and Bad Breath?
There is no possible way in which you can eliminate all the chances of getting affected by a stomach ulcer, you can take certain steps to try to keep things at bay. They include:
Avoid trigger foods.
Not everybody is built the same way, but most people react poorly to spicy or fatty, or acidic foods. Should this happen, you might want to try and avoid these food items to create a surge of acid in your system and skyrocket the chances of developing or resurfacing ulcers.
Limit your consumption of over-the-counter medications.
Should you have to take what we call NSAIDs, it is advisable that you take them post-meal. This mitigates the effects of the medicines in your body and lets the stomach’s natural mechanism function in its own way.
Control your vices.
Try to quit smoking if you can, and limit your alcohol consumption and usage of nicotine and tobacco products as early as possible. These substances can increase your acid levels if you are exposed to too much of them over prolonged periods.
Reduce your stress.
Previously stress was also considered one of the primary factors that play a significant role in the formation of ulcers, which is not completely true. However, it can lead to the production of excess acid in your stomach which can then cause the formation of sores and lesions.
 05 Apr 2023
05 Apr 2023 The Best Foods for a Healthy Smile
You are what you eat- that’s particularly true for your teeth and gums. We are not the only ones who love starchy and sugary food. As it turns out, the bacteria in our mouths like them as well. These bacteria are the ones responsible for gum disease and tooth decay.
Including a variety of nutrient rich food in our diet from all kinds of food groups benefits and promotes healthy gum and teeth. This means you are going to have to maintain a healthy and balanced diet comprising, fruits, vegetables, calcium and protein rich foods.
So, which foods are best for teeth and gum health?
Some of the best foods for strong teeth are fresh fruits and vegetables owing to their high nutritional value and added teeth cleaning benefits.
Then, there’s calcium-rich foods, such as low-fat or fat-free milk, yogurt and cheese, fortified soy milk drinks, tofu, canned salmon, almonds and green leafy vegetables that promote the development of stronger and healthy teeth and bones. Chewing on crunchy foods gets enables the saliva flow, which along with water, helps to rinse away plaque causing bacteria and left over food particles.
Cheese, Milk, and Yogurt
Cheese is one of the best food items for the promotion of healthy teeth for a large number of reasons. Firstly, it is low in sugar content and high in calcium. It contains casein, which is a protein that plays a significant role in fortifying and strengthening the tooth enamel. Cheese is also calcium- rich, which is crucial for the maintenance of a healthy bone density. Cheese is also very high in phosphate content, which balances pH levels in the mouth, which helps in the preservation of the tooth enamel. Another great reason cheese is a friend to our teeth, as mentioned earlier, is that chewing it increases saliva secretion that helps to rinse away bacteria in the mouth.
Besides, good and old fashioned fluoridated water, milk is the best drink when it concerns your teeth. It’s calcium-rich. Milk, like cheese, also lowers and balances the acid levels in the mouth, which enables fighting tooth decay and cavities.
Yogurt is filled with calcium- content and most importantly probiotics that defend you and your teeth against cavities, bad breath and gum disease.
Celery, Carrots, and Other Crunchy Veggies
Vegetables are good for teeth because they require a lot of chewing to. Crunchy foods items that contain lots of water are also known as natural teeth cleaners because they promote the secretion of saliva, which helps to scrape away left-over food particles and bacteria. These fresh and crunchy vegetables are usually also rich in some of the most crucial vitamins and minerals for your oral health.
Celery can also be called nature’s dental floss. The fibrous and crunchy texture makes for a very effective natural teeth cleanser.
In addition to being a storehouse of a lot of nutrients, carrots are also known to fight cavities. Carrots are rich in vitamin C, calcium and keratins, and these also offer dental benefits. Consuming fresh carrots also helps you cleanse your teeth, almost like a natural toothbrush. When combined with your saliva, carrots also help to clean stain-causing bacteria and food particles.
Leafy Greens (Spinach, Lettuce, Kale)
Supremely healthy, leafy greens are packed with calcium, folic acid and umpteen other important vitamins and minerals that your teeth and gums could benefit from. Crunchy and fresh greens in salads and sandwiches also help in cleaning your teeth, gut and overall health.
Apples and Pears
Can an apple a day also keep the dentist away? Probably not, but it can certainly help. Including apples or other hard fibrous fruits in your diet can help clean your teeth and increases the secretion of saliva, which can neutralize corrosive acids like citric and malic acids that are left-over in your mouth. While apple juice with sugar and preservatives might add to the process of tooth decay, fresh apples are less likely to cause trouble inside your mouth. Chewing the fibrous texture of apples, specifically the skin, stimulates your gums, further taking down the number of cavity-causing bacteria and increasing the secretion of saliva.
Unlike many acidic fruits, raw pears are known to neutralize acids in your mouth that promote tooth decay.
Nuts
Nuts can benefit your teeth like none other. They are packed with tons of important nutrients like phosphorus and calcium. Nuts like almonds, Brazil nuts and cashews, which help to defend your mouth against bacteria that cause tooth decay. For instance, peanuts are one of the best source of calcium and vitamin D. Almonds contain good amounts of calcium, which promotes teeth and gum health. Cashews are also known to stimulate saliva and walnuts contain everything from fiber, folic acid, iron, thiamine, magnesium, iron, niacin, vitamin E, vitamin B6, potassium and zinc.
Meats and Fatty Fish
Meats are known to offer some of the most significant nutrients mentioned above, and chewing of meat produces saliva. More saliva is definitely good, because it decreases acidity in your mouth and cleans particles of food that promote tooth decay. Red meat and organic meats are especially helpful. Fatty fish (like salmon), and tofu are rich in minerals like phosphorus, an important for protecting the tooth enamel against erosion and decay
Tea and Coffee
Polyphenols are a category of naturally appearing chemicals that are found in many of the foods and drinks that we consume, including teas, coffee and other associated beverages. They are known to have several health benefits, including their function as antioxidants, which can combat cell damage. They are also effective in subsiding inflammation and helping to fight cancer. Green and black teas are rich in polyphenols and have umpteen number of other health benefits.
Cranberries and Raisins (Fresh or Sugar Free)
Cranberries contain a large amount polyphenols (just like tea) and are known to provide antioxidant benefits. Fresh cranberries are especially effective at disrupting the process of plaque formation. Having said that, you must also know that some packaged and dried or dehydrated cranberries contain a lot of added sugar that isn’t so good for teeth or overall health
 05 Apr 2023
05 Apr 2023 What is dental health and how does it affect pregnancy?
The idea of dental health primarily concerns itself with the health of your mouth, teeth and gums. It is a crucial part of your overall health. If you are either planning to get pregnant, or already pregnant, your oral health also becomes an important part of your prenatal care.
Pregnancy can increase your risk for health issues by manifolds, which includes oral health problems, and these problems can affect your health and the health of the foetus. Some studies have directly linked gum diseases to premature birth, for instance. Premature birth refers to the situation where the delivery of the baby happens much before the estimated time, ie before completion of 37 weeks of pregnancy. Premature babies are way more susceptible to developing health problems and diseases at birth, and later in life when they will grow up completely.
Taking proper care of your mouth, teeth and gums during the span of your pregnancy can ensure that you have a healthy pregnancy, a healthy baby.
How does pregnancy affect your dental health?
Certain changes in your body and bodily functions during pregnancy can affect your teeth and gums. Such as:
Pregnancy can increase the level of certain hormones in your body, like progesterone and oestrogen. These can increase the risk for all kinds of oral health problems in your body.
Pregnancy changes your body, as well as your food habits. It might require you to eat certain food items more during pregnancy, which you might not have eaten otherwise. These food items can lead to affecting your dental or oral health. During pregnancy, some people often develop a condition known as Pica. This condition kind of compels them to eat things that can have adverse effect on their oral health. Large amounts of ice-cream or even non-edible things, for instance.
You might brush and floss your teeth comparatively lesser than you did before you got pregnant. This might possibly be because your gums become tender during pregnancy, for some pregnant people, brushing and flossing can cause them to feel nauseated (making you feel sick in your stomach)
These changes can increase your risk for certain dental problems during pregnancy, including:
Cavities, tooth decay or caries-
These are visible but tiny, decaying and damaged areas on the surface of your teeth. Being pregnant makes you more susceptible to cavities. You might also unwillingly pass the bacteria that causes cavities to your baby during pregnancy and after birth. This is not good for the baby because it can cause problems for your child later in their life.
Mercury-free dental fillings and fillings containing mercury (amalgam or silver fillings)-
It is necessary to get your cavities treated and filled before they spiral out of control. But, if you are pregnant, it is important to get your filled only with mercury free dental fillings. Cavities filled with silver fillings or dental amalgam are capable to threatening the health and wellbeing of your baby. An amalgamation is a chemical blend of different substances, namely chemicals and metals. Dental amalgams usually contain mercury in large quantities. For your reference, mercury is a silvery, shiny and toxic metal, that is also used in the manufacturing of thermometers.
If your body contains mercury in higher quantities inside your body, you are likely to pass it on to the placenta inside your body, or while nursing the baby. Scientific researches have claimed that pregnant people who have been exposed to mercury fillings or mercury in any form are at a higher risk of a miscarriage, preeclampsia and babies with low birth weight, as compared to people who haven’t been exposed to mercury fillings. Mercury also can also harm the functions of the brain, kidneys and other organs.
The US Food and Drug Administration or FDA recommends that you don’t get any dental fillings if you are either pregnant, or even planning to get pregnant. If you do need to get a dental cavity filled, you can ask your dental health expert for a mercury free resin dental filling. This filling is designed to have the same colour as your teeth. It is chemically composed of a type of plastic mixed with powdered glass. Composite resin fillings don’t pose a threat to your health or to the health of your baby, because they don’t contain harmful metals like mercury.
Having said that, the FDA also does not recommend that you get your dental amalgam fillings removed that you already have unless your dentist says that there is an issue with the filling.
Gingivitis.
Gingivitis is the swelling up, inflammation and redness in the gums. If left unattended, it can easily spiral into something way more serious. The hormones secreted in your body during pregnancy can increase your risk of getting gingivitis. It shown that around 60-70% of the people who are pregnant struggle with gingivitis. The tell-tale signs and symptoms of gingivitis include:
- Redness and swelling
- Tenderness in the gums
- Bleeding of the gums, even when you brush your teeth gently
- Shiny gums
Loose teeth.
Higher levels of the hormones like progesterone and oestrogen are secreted in the body during pregnancy. These hormones can temporarily loosen the tissues and bones that keep your teeth in place. This can make your teeth loose.
Periodontal disease (Popularly known as periodontitis or gum disease).
If a situation of gingivitis goes unsupervised, it can cause the gums to suffer from periodontal diseases. This causes serious infection in the gums and troubles the jaw bones that are responsible for holding the teeth in their place. If your teeth get loose, you might as well have to get it extracted or uprooted.
Oral diseases like Periodontitis can also lead to bacteraemia, which is a situation where the bacteria reach the bloodstream. This is a serious condition that needs immediate medical supervision. Smoking can have unfathomable adverse effects on the gums, often leading up to a gum disease.
Pregnancy tumours (also called pyogenic granuloma).
These tumours are not malignant in nature. In other words, they are not cancerous. These are simple lump like structures that form on the gums, especially between the teeth. Pregnancy tumours usually look raw and red, and tend to bleed very easily. These lumpy structures are caused when there is way too much plaque accumulation. For your reference, plaque is a sticky film like formation on the surface of the teeth. These tumours usually go away without needing any severe medical attention, after the baby is born. However, in many rare cases, these tumours have to be removed by a dental health expert.
Tooth erosion
If you are struggling with vomiting tendencies caused by the morning sickness, your teeth might be exposed to way too much stomach acid at regular intervals. This acid might harm the enamel or the hard outer surface of the teeth. Nausea and vomiting of pregnancy (NVP), also popularly known as morning sickness, thankfully, happens only during the first few months of pregnancy.
What are signs and symptoms of dental problems during pregnancy?
If you happen to come across signs or symptoms of a dental illness, seek immediate help from your dental health expert or your prenatal care provider. Signs, however, are different from that of symptoms. Signs of a condition are something that others can see on you, like a rash or swelling. Whereas, a symptom is something that only you will be able to feel or experience, like a lump inside your mouth.
Periodontitis and Adverse Pregnancy Outcomes
There has been way too much discussion in the recent years about the relationship never maternal periodontitis and pregnancy outcomes. While there is no cemented conclusion, an overview of 23 systematically conducted studies through 2016 have concluded that the connection exists between periodontitis and pre-mature or preterm birth, low birthweight babies, and the development of preeclampsia.
Some more research is needed to finalise and seal the deal once and for all. To determine the relationship between periodontitis or gum disease and the pregnancy outcomes. However, should periodontitis start developing during the span of your pregnancy, scaling and root planning is recognized as the safest options to deal with it.
The statement issued by the American College of Obstetricians and Gynaecologists (ACOG) on oral care during pregnancy and for the time after that states that “despite the lack of evidence for a causal relationship between periodontal disease and adverse pregnancy outcomes, the treatment of maternal periodontal disease during pregnancy is not associated with any adverse maternal or birth outcomes,” and “prenatal periodontal therapy is associated with the improvement of maternal oral health.”
Signs and symptoms of dental problems include:
- Bad breath
- Loosening of teeth
- Mouth sores or lumps on the gums
- Increased gaps between your teeth
- Receding gums
- Accumulation of pus along your gumline
- Red, swollen, tender or shiny; or bleeding gums.
- Toothache
If you are experiencing a sharp pain or swelling, it is recommended that you fix an appointment with your dental health expert right away. If you seem to have a dental infection, you need quick treatment to help prevent it from reaching your baby.
How can you prevent dental problems during pregnancy?
Go for dental check-ups at regular intervals before and during pregnancy. During your visits, you might want to talk to your dentists about:
If you’re pregnant or are looking forward to get pregnant.
Talk to him about the medicines you take. This includes every medicine from prescription drugs to over the counter drugs, health supplements and everything else.
Let him know if your pregnancy is high-risk. High-risk simply means that you, your baby or maybe both of you are at an increased risk for problems during pregnancy. Your pregnancy may be high-risk if you happen to be struggling with a chronic health condition, you have complications from your previous pregnancy or if you are struggling with some other health conditions that can have an adverse effect on your health or the health of your baby.
If your prenatal care provider has specifically spoken to you about your oral health.
We cannot emphasise enough on the importance of being under regular dental check-ups before and during pregnancy, so your dentist can look for and cure your dental problems at the earliest. Regular teeth cleaning procedures can help you keep your teeth and gums healthy.
Are dental X-rays safe during pregnancy?
X-rays are an important part of a regular dental check-up. They can throw light at the impending dental issues, or issues with your gums and jaws, and nip them at the bud. An X-ray is a medical test that makes use radiation to take a picture on film. Radiation energy that can be harmful to your health if you’re exposed to it for longer periods of time.
To answer your question, dental X-rays are safe during pregnancy. This procedure uses very small amounts of radiations, and your dental health expert will possibly cover you with a special apron or sheet, and collar you to protect your baby and you. However, should you need an X-ray, make sure that your dental health expert is aware of your pregnancy or that you are looking forward to it.
How are dental problems treated during pregnancy?
If you are struggling with a dental or oral ailment that requires immediate medical attention, make sure that your dental health knows about your pregnancy. Based on your condition and the stage of pregnancy you’re in, you might also have to get the dental ailment treated. Treatments that are safe during pregnancy include:
Medicine, including pain killers and antibiotics to treat infections.Should you need any medication, your dentist will prescribe something that is safe for you and the baby. Again, you can talk to your prenatal caregiver about the medicines that your dental health expert might have prescribed. It would be wise to not consume any medicine without consulting with your prenatal care giver.
What can you do to help prevent dental problems?
Here’s how you can help keep your teeth and gums healthy:
Maintain a healthy dental and oral hygiene regimen by brushing your teeth with fluoride toothpaste twice a day and floss once a day. Use a toothbrush with soft bristles. Regular brushing and flossing can remove plaque and help keep your teeth and gums healthy.
If you cannot seem to brush your teeth because of the morning sickness or nausea , try using antacids or rinse your mouth with a mixture of 1 teaspoon baking soda in a cup of water. Rinsing can help you deal with the amount of acid in your mouth. Antacids, as the name suggests, help neutralize stomach acid. You can conveniently get them over the counter without a prescription from your nearest pharmacy. But don’t consume any medicine—even the ones that you can obtain OTC—without consulting your prenatal care provider.
Visit your dentist at regular intervals for your dental check-up (twice a year), even during pregnancy. During the visit, inform your dentist about your pregnancy.
Get into the habit of a healthy and clean diet, and most importantly limit the intake of sweet or sugary food items. Healthy food items include fruits and vegetables, meat with low fat content, whole grain breads , pasta and low fat or toned daily products. Replace sugary beverages with water or fresh juice. Eating heathy food items provides you and your baby with all kinds of important nutrients. Your baby’s teeth start developing between 3 and 6 months of pregnancy. Nutrients like calcium, protein, phosphorus, and vitamins A, C and D, help your baby’s teeth grow healthy.
If you’re craving things like large amounts of ice, paste or dirt, discuss it with your prenatal care provider.
Quit smoking. If you need help to quit, consult your prenatal care provider.
Conclusion
Pregnancy can significantly increase the risk of oral health conditions such as Gingivitis and dental caries. It is recommended that you consult both your obstetrician and dentist on the importance of good oral hygiene throughout the pregnancy and post-partum. Should you require regular or emergency dental care, including the use of local anaesthetics and radiographs are safe for both the mother and the foetus.
